Rheumatoid arthritis is a chronic arthritic condition of the joints. Like osteoarthritis, rheumatoid arthritis causes joint pain, swelling and stiffness. Yet, rheumatoid arthritis and osteoarthritis are very different conditions. While osteoarthritis is thought of as a disease of wear and tear, rheumatoid arthritis is an autoimmune disease. This means that instead of protecting the body, the immune system turns on its own body tissues. In the case of rheumatoid arthritis, the immune system attacks the joints. And most at risk are the small joints of the hands, feet and wrists.
In developed countries such as the UK, around 1% of the population may have rheumatoid arthritis. It is a condition that tends to run in families, and it affects around three times as many women as men.
It is important to understand the underlying causes and triggers for a condition like rheumatoid arthritis. This understanding means that we might be able to prevent disease progression or even reverse it. So this is an important part of the research into rheumatoid arthritis and other autoimmune diseases.
Scientists searching for the cause of rheumatoid arthritis believe that bacteria play an important part. In particular, at least for rheumatoid arthritis, studies implicate certain types of bacteria that cause urinary tract infections.
Bacteria and UTIs
Escherichia coli (E. coli) bacteria cause the majority of urinary tract infections. These bacteria tend to colonise the bladder and cause cystitis. In contrast, Proteus bacteria such as Proteus mirabilis invade the upper parts of the urinary tract, such as the ureters, the tubes leading from the kidney to the bladder, as well as the kidney itself. Proteus bacteria cause around 10 to 15% of urinary tract infections. Though the infections may be chronic, low-grade infections without obvious symptoms.
Proteus and some other disease-causing bacteria, but not E. coli, produce an enzyme called urease. This enzyme helps them invade, colonise and spread. The urease made by Proteus bacteria is toxic to the body’s tissues. What’s more, scientists believe urease has a role in the development of rheumatoid arthritis. It may also encourage the formation of urinary stones. In addition, it helps the Proteus bacteria to hide from the immune system and from antibiotic medication.
Antibodies and molecular mimicry
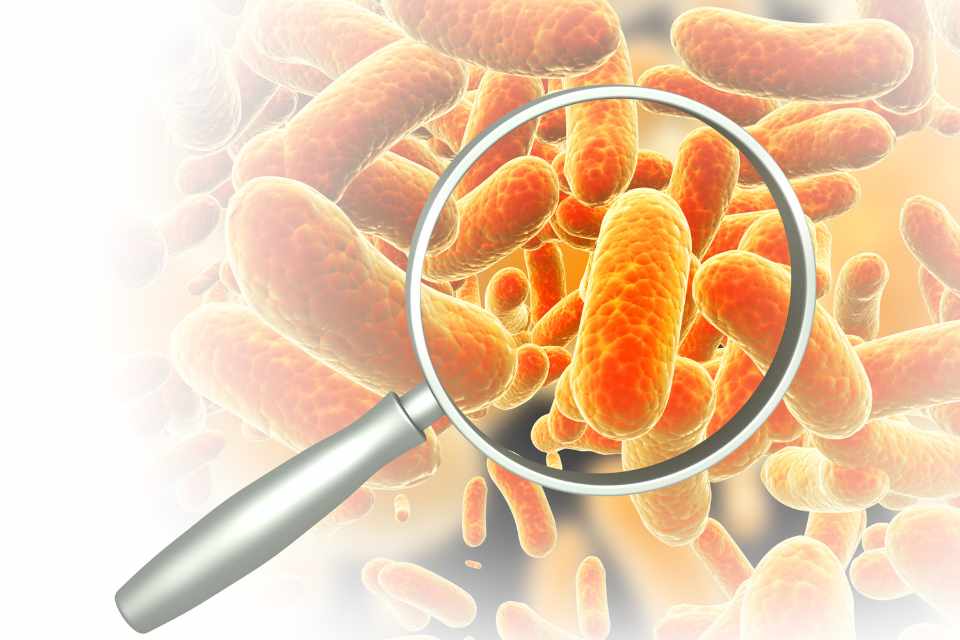
Proteus bacteria can cause long term infections of the urinary tract. When the immune system detects an infection it creates antibodies to destroy foreign proteins such as bacteria. But urease is also a protein. So, in long-lasting urinary tract infections, the immune system can produce antibodies to urease. What scientists now know, is that in some people, the urease antibodies may also destroy cartilage.
This autoimmune process is called molecular mimicry. To the antibodies, the protein sequences of the membranes and collagen look a lot like those of an invader. So, the antibodies attack and destroy the joint membranes and cartilage. This can cause chronic inflammation and destruction or deformity of the joints.
If the Proteus infections are recurrent or chronic, this just adds fuel to the fire. So that, chronic UTIs can perpetuate the autoimmune condition.
Who is most at risk?
We know that women are more at risk for urinary tract infections than men. The researchers suggest that this along with their findings also explains why more women than men suffer from rheumatoid arthritis.
Interestingly, many herbs that were used traditionally for symptoms of urinary tract infections are also traditional remedies for arthritis or rheumatic conditions. Take juniper (Juniperus communis) for example, with a reputation for notable anti-inflammatory and anti-rheumatic effects, as well as antibacterial and antimicrobial activity. In fact, in studies, Juniper has been found effective against Proteus mirabilis in vitro. This could perhaps explain why complementary and alternative medicine therapies are popular in people with rheumatoid arthritis worldwide.
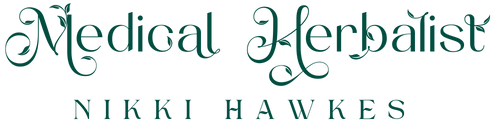





0 Comments