A diagnosis of fibromyalgia means you are most likely a woman between the ages of 20 and 50. You are also likely to also suffer with irritable bowel syndrome. Fibromyalgia and irritable bowel syndrome often occur together. Not everyone with irritable bowel syndrome has fibromyalgia. But most people with fibromyalgia do have irritable bowel syndrome.
Irritable bowel syndrome is a condition of abdominal pain with altered bowel habit. Whilst fibromyalgia is a condition of chronic generalised and focal muscular pain. Is it possible these seemingly different conditions have a common cause?
The current medical view is that fibromyalgia has no known cause. In conventional medicine it is often believed to be ‘all in the mind’. But, new research suggests a link between fibromyalgia and irritable bowel syndrome. This is another condition that used to be considered psychological rather than physiological. We now know that in the majority of cases irritable bowel syndrome is due to bacterial overgrowth in the small intestine.
The pain and stiffness of fibromyalgia occur in multiple places. Specifically, in the neck, shoulders, elbows, knees, lower back and hips. The pain can be severe and is made worse by stress or exertion.
In addition, people with fibromyalgia have other associated symptoms. Such as fatigue and headaches, especially of the migraine type. Numbness, poor sleep pattern, memory problems and difficulty thinking clearly are common. And, typically there will be digestive problems like irritable bowel syndrome.
Your doctor focuses on minimising your symptoms with analgesics and antidepressants. But they would generally not look for underlying causes or offer any hope of a cure. The prescribed medications are only effective for the minority of fibromyalgia sufferers. They also have side effects of their own.
From a functional medicine perspective, chronic diseases are due to chronic dysfunction. So a functional medicine practitioner looks for an underlying cause.
On examination fibromyalgia muscle tissue is different to healthy muscle tissue. The differences cause reduced cellular energy production and reduced blood flow to the muscles. These changes can result in an increased perception of pain and fatigue.
Other common findings are below normal levels of magnesium and vitamin D deficiency and low levels of tryptophan. When tryptophan is low, the production of serotonin and melatonin is also reduced. Serotonin is the feel-good hormone, so a deficiency in this hormone can lead to symptoms such as anxiety and depression. Whilst melatonin is the sleep hormone. A deficiency of melatonin can result in sleep problems.
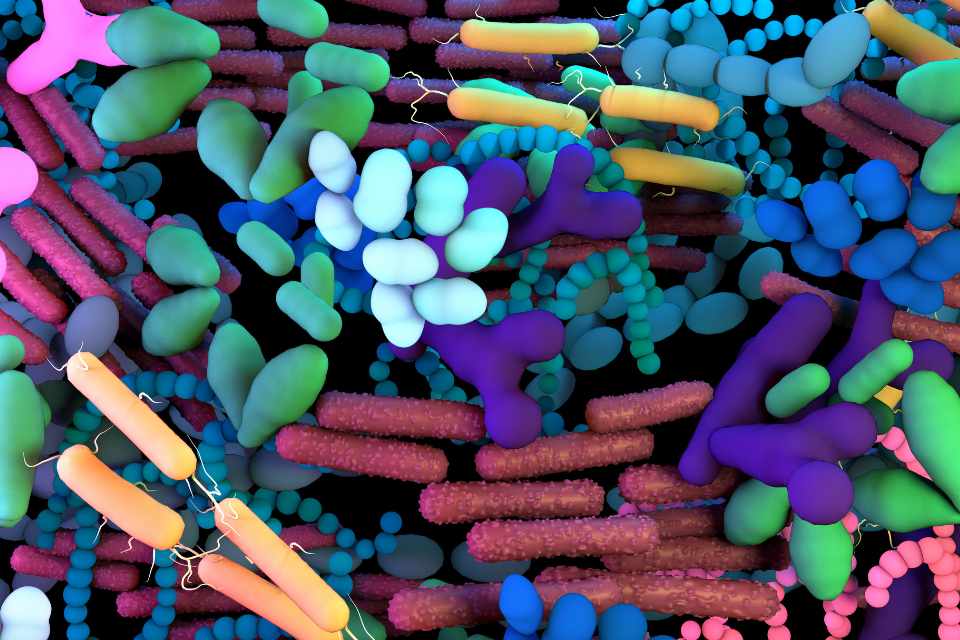
A recent study of fibromyalgia sufferers discovered that all had small intestinal bacterial overgrowth. The severity of their fibromyalgia correlated with the degree of bacterial overgrowth. We now know that most irritable bowel syndrome is also caused by bacterial overgrowth in the small intestine. So, is it possible that bacterial overgrowth causes both irritable bowel syndrome and fibromyalgia?
As well as changes to bowel function, bacterial overgrowth also changes the sensitivity of nerves supplying the gut wall. It is believed that toxins produced by bacteria can cause hypersensitivity of these nerves. This leads to an increased perception of pain in the abdomen. Such as is experienced with irritable bowel syndrome.
One theory is that in fibromyalgia, gut bacteria toxins may cause generalised hypersensitivity. With increased sensitivity to pain in the muscle fibres, leading to tender, sore muscles.
Restoring a healthy gut function could be key to eliminating the underlying causes of fibromyalgia. Medicinal herbs, dietary changes and or lifestyle changes are a great way to improve gut health.
If you liked this post you might also like:
Are you happy with your current irritable bowel syndrome treatment?






0 Comments